Page 20 - ISAKOS 2020 Newsletter Volume 2
P. 20
CURRENT CONCEPTS
Case Corner: Young Patient
with Femoral Head Limited Subchondral Collapse and Possible Impingement Symptoms
How would you address this case with the ultimate goal of joint preservation in a young active female?
1. Is there any reproducible surgery to address the lesioned area in order to restore femoral head convexity and joint congruity?
2. Would you consider arthroscopic intervention for head- neck junction decompression because of the impingement symptoms (currently less pain during walking and more
Patient
Iftach Hetsroni, MD, Associate Prof. pain on FADIR testing)?
Meir General Hospital, Kfar Saba, and Sackler Faculty of Medicine Tel Aviv University, ISRAEL
3. What is the likelihood that this treatment could lead to substantial long-term improvement?
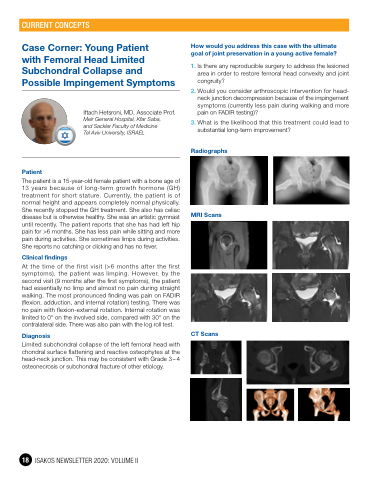
Radiographs
MRI Scans
CT Scans
The patient is a 15-year-old female patient with a bone age of 13 years because of long-term growth hormone (GH) treatment for short stature. Currently, the patient is of normal height and appears completely normal physically. She recently stopped the GH treatment. She also has celiac disease but is otherwise healthy. She was an artistic gymnast until recently. The patient reports that she has had left hip pain for >6 months. She has less pain while sitting and more pain during activities. She sometimes limps during activities. She reports no catching or clicking and has no fever.
Clinical findings
At the time of the first visit (>6 months after the first symptoms), the patient was limping. However, by the second visit (9 months after the first symptoms), the patient had essentially no limp and almost no pain during straight walking. The most pronounced finding was pain on FADIR (flexion, adduction, and internal rotation) testing. There was no pain with flexion-external rotation. Internal rotation was limited to 0° on the involved side, compared with 30° on the contralateral side. There was also pain with the log roll test.
Diagnosis
Limited subchondral collapse of the left femoral head with chondral surface flattening and reactive osteophytes at the head-neck junction. This may be consistent with Grade 3–4 osteonecrosis or subchondral fracture of other etiology.
18 ISAKOS NEWSLETTER 2020: VOLUME II