Page 22 - ISAKOS 2020 Newsletter Volume 2
P. 22
CURRENT CONCEPTS
Young Patient with Femoral Head Limited Subchondral Collapse and Possible Impingement Symptoms
At 1 year, magnetic resonance imaging (MRI) is used to assess for adequate healing and creeping substitution of the graft before the patient returns to more vigorous activities. At the time of the latest follow-up, our patient (the 15-year-old male patient with intraoperative photographs) was pain-free and had returned to running and heavy squats. The results of our procedure need to be followed closely and compared with those of other treatments, but we believe that our approach has been a successful option for young patients with osteonecrosis of the femoral head and secondary subchondral collapse.
Hajime Utsunomiya, MD, PhD
This is a challenging case in a female gymnastic athlete. In my opinion, this is a typical case of subchondral insufficiency fracture of the femoral head (SIFFH). The T2-weighted MRI scan shows a high-signal band at the femoral head. The most important finding is that the band is parallel to the subchondral area along the femoral head. I believe that the classic findings of SIFFH are a diffuse femoral head bone-marrow edema pattern and an irregular / serpiginous subchondral band. Proton or T1-weighted MRI will be required to diagnose it firmly.
As for the treatment options, conservative treatment has to be the first choice. Although the left hip symptoms have improved, arthroscopic management must be considered for several reasons. First, associated labral injury could be the cause of SIFFH. We have reported that SIFFH is highly associated with labral tearing. Second, arthroscopic surgery is beneficial to directly diagnose the cartilage state in a patient with SIFFH. Third, SIFFH can be fixed by means of arthroscopic internal fixation with use of hydroxyapatite- poly-L-lactic acid (HA / PLLA) pins (Fig. 2). Please refer to our article regarding the arthroscopic classification and treatment of SIFFH (Uchida and Utsunomiya et al., KSSTA 2018). Fourth, the reactive osteophytes at the head-neck junction are severe enough to cause impingement and limit the range of internal rotation. Given these considerations, the best treatment option in this case would be (1) arthroscopic evaluation of SIFFH, (2) internal fixation of SIFFH with use of an HA / PLLA pin, if necessary, (3) labral repair, if necessary, (4) cam osteochondroplasty, and (5) capsular plication.
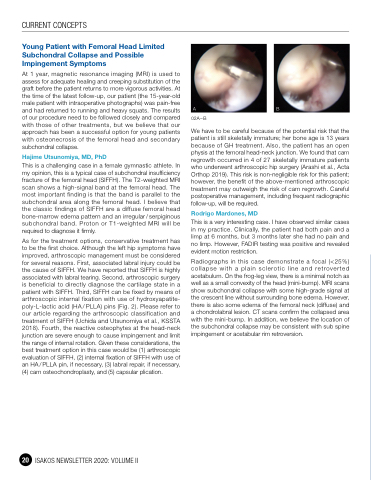
AB
02A–B
We have to be careful because of the potential risk that the patient is still skeletally immature; her bone age is 13 years because of GH treatment. Also, the patient has an open physis at the femoral head-neck junction. We found that cam regrowth occurred in 4 of 27 skeletally immature patients who underwent arthroscopic hip surgery (Arashi et al., Acta Orthop 2019). This risk is non-negligible risk for this patient; however, the benefit of the above-mentioned arthroscopic treatment may outweigh the risk of cam regrowth. Careful postoperative management, including frequent radiographic follow-up, will be required.
Rodrigo Mardones, MD
This is a very interesting case. I have observed similar cases in my practice. Clinically, the patient had both pain and a limp at 6 months, but 3 months later she had no pain and no limp. However, FADIR testing was positive and revealed evident motion restriction.
Radiographs in this case demonstrate a focal (<25%) collapse with a plain sclerotic line and retroverted acetabulum. On the frog-leg view, there is a minimal notch as well as a small convexity of the head (mini-bump). MRI scans show subchondral collapse with some high-grade signal at the crescent line without surrounding bone edema. However, there is also some edema of the femoral neck (diffuse) and a chondrolabral lesion. CT scans confirm the collapsed area with the mini-bump. In addition, we believe the location of the subchondral collapse may be consistent with sub spine impingement or acetabular rim retroversion.
20 ISAKOS NEWSLETTER 2020: VOLUME II