Page 43 - ISAKOS 2020 Newsletter Volume 2
P. 43
CURRENT CONCEPTS
However, QT autografts offer a substantial range of advantages that have led to their re-emergence. Specifically, QT grafts can be reliably templated from preoperative magnetic resonance imaging (MRI) scans (Fig. 1); harvested in an open, mini-open, or arthroscopic- assisted / minimally invasive fashion1; (3) harvested as a full or partial-thickness graft, with or without a bone block (Fig. 2); used with a host of available fixation options; and (4) prepared for a single-bundle or double-bundle technique. Moreover, QT grafts are amenable to transtibial, anatomical, and / or all-inside techniques. Given these proposed advantages, an evidence-based approach can be used to guide their adoption.
01 Midsagittal MRI scan of an ACL-deficient knee, used for preoperative templating of a QT graft. QT thickness is measured 3 cm proximal
to the proximal pole of the patella. In this case, the thickness was templated at 9.8 mm, compared with the 6.1-mm patellar tendon.
The >600 peer-reviewed publications on the topic—a third of which have been published within the past 5 years—are evidence that the QT is gaining popularity2. In fact, this topic has facilitated the formation of the International Quadriceps Tendon Interest (IQTI) Group, the main objective of which is to globally disseminate clinical and research expertise regarding the use of the QT for knee ligament procedures.
However, there remains an undetermined learning curve associated with harvest and preparation that may pose a barrier to broader implementation. From an evidence perspective, surgeons should take comfort in a recent, methodologically sound meta-analysis of 27 studies involving 2,856 ACL patients, which demonstrated comparable clinical and functional outcomes and graft survival rates in comparison with BPTB and HT autografts3.
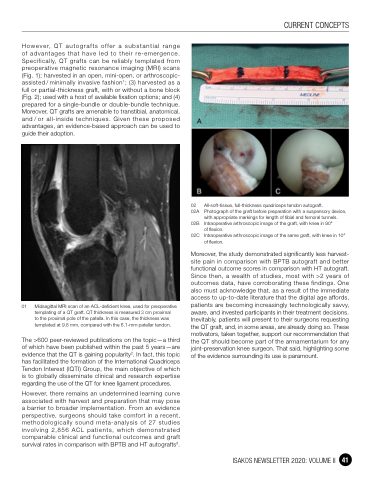
02 All-soft-tissue, full-thickness quadriceps tendon autograft.
02A Photograph of the graft before preparation with a suspensory device,
with appropriate markings for length of tibial and femoral tunnels.
02B Intraoperative arthroscopic image of the graft, with knee in 90°
of flexion.
02C Intraoperative arthroscopic image of the same graft, with knee in 10°
of flexion.
Moreover, the study demonstrated significantly less harvest- site pain in comparison with BPTB autograft and better functional outcome scores in comparison with HT autograft. Since then, a wealth of studies, most with >2 years of outcomes data, have corroborating these findings. One also must acknowledge that, as a result of the immediate access to up-to-date literature that the digital age affords, patients are becoming increasingly technologically savvy, aware, and invested participants in their treatment decisions. Inevitably, patients will present to their surgeons requesting the QT graft, and, in some areas, are already doing so. These motivators, taken together, support our recommendation that the QT should become part of the armamentarium for any joint-preservation knee surgeon. That said, highlighting some of the evidence surrounding its use is paramount.
ISAKOS NEWSLETTER 2020: VOLUME II 41