Page 17 - ISAKOS 2021 Newsletter Volume 1
P. 17
The Eeklo Subvastus Approach for Total Knee Arthroplasty Detailed Surgical Technique
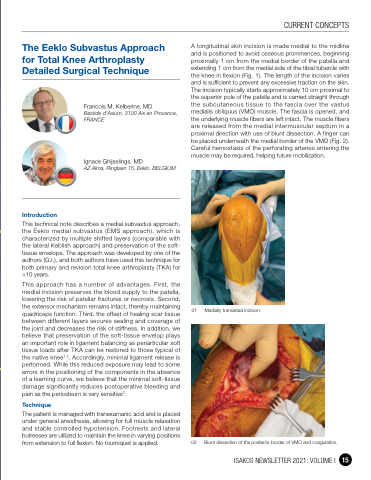
A longitudinal skin incision is made medial to the midline and is positioned to avoid osseous prominences, beginning proximally 1 cm from the medial border of the patella and extending 1 cm from the medial side of the tibial tubercle with the knee in flexion (Fig. 1). The length of the incision varies and is sufficient to prevent any excessive traction on the skin. The incision typically starts approximately 10 cm proximal to the superior pole of the patella and is carried straight through the subcutaneous tissue to the fascia over the vastus medialis obliquus (VMO) muscle. The fascia is opened, and the underlying muscle fibers are left intact. The muscle fibers are released from the medial intermuscular septum in a proximal direction with use of blunt dissection. A finger can be placed underneath the medial border of the VMO (Fig. 2). Careful hemostasis of the perforating arteries entering the muscle may be required, helping future mobilization.
01 Medially translated incision.
02 Blunt dissection of the posterior border of VMO and coagulation.
Introduction
Francois M. Kelberine, MD
Bastide d’Axium, 3100 Aix en Provence, FRANCE
Ignace Ghijselings, MD
AZ Alma, Ringlaan 15, Eeklo, BELGIUM
This technical note describes a medial subvastus approach, the Eeklo medial subvastus (EMS approach), which is characterized by multiple shifted layers (comparable with the lateral Keblish approach) and preservation of the soft- tissue envelope. The approach was developed by one of the authors (G.I.), and both authors have used this technique for both primary and revision total knee arthroplasty (TKA) for >10 years.
This approach has a number of advantages. First, the medial incision preserves the blood supply to the patella, lowering the risk of patellar fractures or necrosis. Second, the extensor mechanism remains intact, thereby maintaining quadriceps function. Third, the offset of healing scar tissue between different layers secures sealing and coverage of the joint and decreases the risk of stiffness. In addition, we believe that preservation of the soft-tissue envelop plays an important role in ligament balancing as periarticular soft tissue loads after TKA can be restored to those typical of the native knee1,2. Accordingly, minimal ligament release is performed. While this reduced exposure may lead to some errors in the positioning of the components in the absence of a learning curve, we believe that the minimal soft-tissue damage significantly reduces postoperative bleeding and pain as the periosteum is very sensitive3.
Technique
The patient is managed with tranexamanic acid and is placed under general anesthesia, allowing for full muscle relaxation and stable controlled hypotension. Footrests and lateral butresses are utilized to maintain the knee in varying positions from extension to full flexion. No tourniquet is applied.
CURRENT CONCEPTS
ISAKOS NEWSLETTER 2021: VOLUME I 15