Page 32 - ISAKOS 2018 Newsletter Volume 2
P. 32
CURRENT CONCEPTS
There are two common osseous root-fixation techniques: the bone bridge technique and the bone plug technique. The bone bridge MAT technique has strong time-zero fixation as the relationship between the anterior and posterior meniscal roots is maintained. This technique has some disadvantages, including the loss of bone stock, the difficulty of dealing with graft-size mismatch, and the technical challenge of “flipping” the meniscus into place.
Update on Meniscal Allograft Transplantation
The traditional bone plug MAT technique is bone stock- preserving. It also is easier to accommodate graft-size mismatch. There is no required “flipping” of the meniscal transplant as there is with the bone bridge technique. Nevertheless, this technique is associated with several challenges and disadvantages, including a lack time-zero fixation strength, the challenge of seating plugs with a depth of 8 mm to 10 mm, and a difficulty in the lateral compartment due to close proximity of the lateral meniscal root insertions and the risk of tunnel overlap.
Evolving techniques seek to combine the most favorable aspects of the three standard root-fixation strategies.
03
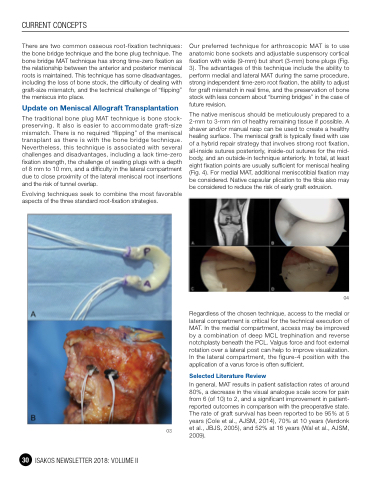
Our preferred technique for arthroscopic MAT is to use anatomic bone sockets and adjustable suspensory cortical fixation with wide (9-mm) but short (3-mm) bone plugs (Fig. 3). The advantages of this technique include the ability to perform medial and lateral MAT during the same procedure, strong independent time-zero root fixation, the ability to adjust for graft mismatch in real time, and the preservation of bone stock with less concern about “burning bridges” in the case of future revision.
The native meniscus should be meticulously prepared to a 2-mm to 3-mm rim of healthy remaining tissue if possible. A shaver and/or manual rasp can be used to create a healthy healing surface. The meniscal graft is typically fixed with use of a hybrid repair strategy that involves strong root fixation, all-inside sutures posteriorly, inside-out sutures for the mid- body, and an outside-in technique anteriorly. In total, at least eight fixation points are usually sufficient for meniscal healing (Fig. 4). For medial MAT, additional meniscotibial fixation may be considered. Native capsular plication to the tibia also may be considered to reduce the risk of early graft extrusion.
04
Regardless of the chosen technique, access to the medial or lateral compartment is critical for the technical execution of MAT. In the medial compartment, access may be improved by a combination of deep MCL trephination and reverse notchplasty beneath the PCL. Valgus force and foot external rotation over a lateral post can help to improve visualization. In the lateral compartment, the figure-4 position with the application of a varus force is often sufficient.
Selected Literature Review
In general, MAT results in patient satisfaction rates of around 80%, a decrease in the visual analogue scale score for pain from 6 (of 10) to 2, and a significant improvement in patient- reported outcomes in comparison with the preoperative state. The rate of graft survival has been reported to be 95% at 5 years (Cole et al., AJSM, 2014), 70% at 10 years (Verdonk et al., JBJS, 2005), and 52% at 16 years (Wal et al., AJSM, 2009).
30 ISAKOS NEWSLETTER 2018: VOLUME II