Page 37 - Layout 1
P. 37
CURRENT CONCEPTS
Advanced imaging modalities including computed Conclusion
tomography (CT) (Figure 3, 4, 5) and magnetic resonance Differentiation between classic (inferior) versus superior
imaging (MRI) have been reported to demonstrate accurate Bennett lesions and whether the lesion is attached or a
localization of the lesions. These studies can more readily free fragment is important when treating the overhead
identify a calcification adjacent to the posterior glenoid or thrower. Furthermore, “pitcher’s mound” lesions have
in the adjacent capsular tissues. Theoretically, MRI offers also been reported in the posterosuperior region, but are
the advantage of evalauation of the shoulder joint, although arguably a misnomer, as no patient described was under
a small bony lesion could be interpreted as labrum in this
52 years, nor were any baseball players. There are enough
region.
differences in the current Bennett’s lesion literature with
Treatment
regards to location, presentation, and treatment options
that careful consideration of the patients’ functional level,
The treatment of a Bennett lesion remains debatable.
Determining a course of action is further complicated by concomitant shoulder pathology, and etiology of pain should
be considered prior to counseling a patient regarding their
reviewing the results of classic (inferior) lesions versus superior conservative and surgical options.
Bennett lesions, and free fragments versus subperiosteal
or attached osteophytic lesions. Treatment is initially
conservative with stretching of the posterior capsule and
strengthening of the external rotators. None of the twelve
pitchers identified in the Wright and Paletta study required
surgical intervention for the lesion during their time with the
respective baseball organization. Two of the twelve (17%) did
require time on the disabled list; however, neither individual
had symptoms or complaints of posterior shoulder pain.
Early accounts for management encouraged open resection;
however, conservative management was later advocated
as early surgical results were poor. There are many reports
detailing both open and arthroscopic resection of the 03 04
Bennett’s lesion with varying results. Currently, a failure of
conservative management, with an inability to return to
asymptomatic throwing, warrants arthroscopic intervention.
Addressing the associated pathology and not the Bennett
lesion proper has been proposed, however, there have
been reports of arthroscopic removal of the isolated Bennett
lesions in patients with pain while throwing which resulted
in complete relief of symptoms. Review of these particular
studies is beyond the scope of this review; however, upon
successful resection of the lesion, additional technical
considerations remain. These include: leaving the capsule
in situ, repairing the capsule to the labrum, repairing the
capsule side to side, shifting excess capsule superiorly, or
repairing the capsule and the labrum to the glenoid with
suture anchors. Further concern exists when dealing with
05
throwing athletes, chiefly baseball players. Over-tightening of
the posterior capsule could inhibit full external rotation and be
detrimental to velocity compromising their ability to compete.
01 Images of the various types of Bennett lesions described in
the literature: avulsed posteroinferior lesion (1A) subperiosteal
posteroinferior lesion (1B) avulsed posterosuperior lesion (1C) attached
posterosuperior lesion (“Pitcher’s Mound”) (1D).
02 Plain film axillary view demonsrating possible osseous change in the
posterior glenoid.
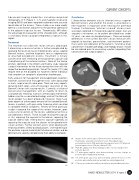
03 CT arthrogram sagittal view demonstrating osseous change on
posterior glenoid appearing attached.
04 CT arthrogram axial view demonstrating a Bennett lesion on the
posterior glenoid attached, but possibly becoming fragmented.
05 CT bony reconstructions with posteroinferior attached Bennett lesion.
02
ISAKOS NEWSLETTER 2014: Volume II 35